
U.S. Health Innovation Ecosystem: A Historical Overview
The U.S. health innovation ecosystem stands as a global benchmark, showcasing the successful collaboration between public and private sectors in advancing biomedical research and technology. This dynamic landscape emerged significantly during World War II, with pivotal government-supported initiatives like the mass production of penicillin, which revolutionized medical treatment and set the stage for subsequent healthcare breakthroughs. Insights gained from federal funding for biomedical research have fueled innovative partnerships, leading to discoveries that benefit both military and civilian populations. The historical context highlights how the foundations laid during wartime efforts continue to drive contemporary advancements in medicine through strategic public-private partnerships. As we navigate the complexities of modern healthcare, understanding this intricate ecosystem is essential to promoting sustainable innovation and ensuring continued progress in the field.
The landscape of U.S. healthcare innovation embodies a rich tapestry of ideas and collaborations that have shaped modern biomedicine. Often referred to as the biomedical ecosystem, this intricate web consists of partnerships between educational institutions, government agencies, and private enterprises, each playing a crucial role in fostering scientific discovery. Since the 1940s, federal investment in research has harmoniously blended with entrepreneurial spirit, enabling remarkable technological advancements that have transformed patient care. This synergy not only reflects the storied history of American biomedical research but also highlights a broader paradigm where strategic alliances cultivate a flourishing environment for innovative medical solutions. By embracing a legacy rooted in public investment and cooperative research, the U.S. continues to lead the way in health innovation.
The Origins of the U.S. Health Innovation Ecosystem
The U.S. health innovation ecosystem is built on a rich history that dates back to World War II, when the urgent demands of wartime propelled significant advancements in biomedical science. Initially, the federal government recognized the necessity of harnessing civilian scientists to pioneer technological breakthroughs. This collaboration between government and academia catalyzed a shift towards a more structured research environment, laying the foundation for modern biomedical innovation. Today, this ecosystem stands as a global leader in scientific advancement, owing much to its historical roots.
The pivotal time of World War II illustrated the critical need for effective medical treatments, particularly as infectious diseases posed serious risks to military personnel. The establishment of entities like the Office of Scientific Research and Development (OSRD) enabled a coordinated effort to channel resources and expertise into developing life-saving solutions. This set the stage for the future growth of the National Institutes of Health (NIH) and other research institutions that form the backbone of the U.S. health innovation system today.
Frequently Asked Questions
What is the role of public-private partnerships in the U.S. health innovation ecosystem?
Public-private partnerships have been a cornerstone of the U.S. health innovation ecosystem, facilitating collaboration between government entities, academic institutions, and private industry. This collaborative dynamic has enabled significant advancements in biomedical innovation, ensuring that research initiatives are well-funded and effectively translated into practical medical solutions.
How has federal funding impacted the U.S. health innovation ecosystem?
Federal funding has been instrumental in shaping the U.S. health innovation ecosystem, particularly in biomedical research. It provides essential financial resources that support academic institutions and industry collaborations, facilitating the discovery of new treatments and technologies essential for public health.
What was the significance of USDA penicillin production during World War II for the U.S. health innovation ecosystem?
The USDA’s mass production of penicillin during World War II marked a pivotal moment in the U.S. health innovation ecosystem. It demonstrated the effectiveness of federal support for biomedical innovation, resulting in the rapid development and distribution of antibiotics that saved countless lives and laid the groundwork for modern pharmaceuticals.
What is the historical context of biomedical innovation in the U.S.?
The history of biomedical innovation in the U.S. traces back to World War II, when urgent health needs prompted government-university partnerships that significantly advanced medical research. This collaboration set the stage for the modern U.S. health innovation ecosystem, characterized by robust funding, research advancements, and effective public-private partnerships.
How did World War II influence the development of the U.S. health innovation ecosystem?
World War II catalyzed the development of the U.S. health innovation ecosystem by highlighting the need for rapid biomedical advancements. Initiatives such as the Office of Scientific Research and Development established collaborative frameworks between the government and research institutions, leading to notable innovations like penicillin and a lasting legacy in biomedical research.
What are the challenges currently facing the U.S. health innovation ecosystem?
Currently, the U.S. health innovation ecosystem faces challenges including proposed cuts to federal funding for biomedical research, which could threaten public-private partnerships that drive innovation. These challenges underscore the importance of sustaining investments in health research to maintain the efficacy and growth of this vital ecosystem.
Why is the U.S. health innovation ecosystem considered a global benchmark?
The U.S. health innovation ecosystem is regarded as a global benchmark due to its successful integration of federal funding, academic research, and private industry. This model has inspired similar systems worldwide, showcasing its effectiveness in generating groundbreaking biomedical innovations and responding to complex health challenges.
| Key Points | Details |
|---|---|
| Historical Origin | The U.S. health innovation ecosystem began during World War II with government-supported research initiatives. |
| Public-Private Partnership | This partnership fostered collaboration between the federal government, academic institutions, and private industries, leading to significant advancements in biomedicine. |
| Impact of WWII | The war highlighted the urgent need for innovations in health technologies, spurring the development of critical medical advancements like penicillin. |
| Role of the NIH | The National Institutes of Health played a crucial role in funding and developing research institutions post-war. |
| Challenges and Funding | Federal funding has come under scrutiny, with potential cuts threatening the ongoing success of the health innovation ecosystem. |
| Legacy and Future | The foundational efforts during the war led to a global benchmark for biomedicine, which must be preserved to sustain further innovation. |
Summary
The U.S. health innovation ecosystem stands as a global exemplar, having evolved from critical wartime collaborations into a cornerstone of modern medical advancements. The partnership between federal institutions, academia, and private industry has fostered significant breakthroughs in biomedicine, particularly evident during World War II with the mass production of penicillin. However, current challenges regarding federal funding highlight the need for ongoing support to maintain this successful model. Preserving the synergies developed over decades is essential for future health innovations and maintaining the progressive momentum of the U.S. health innovation ecosystem.
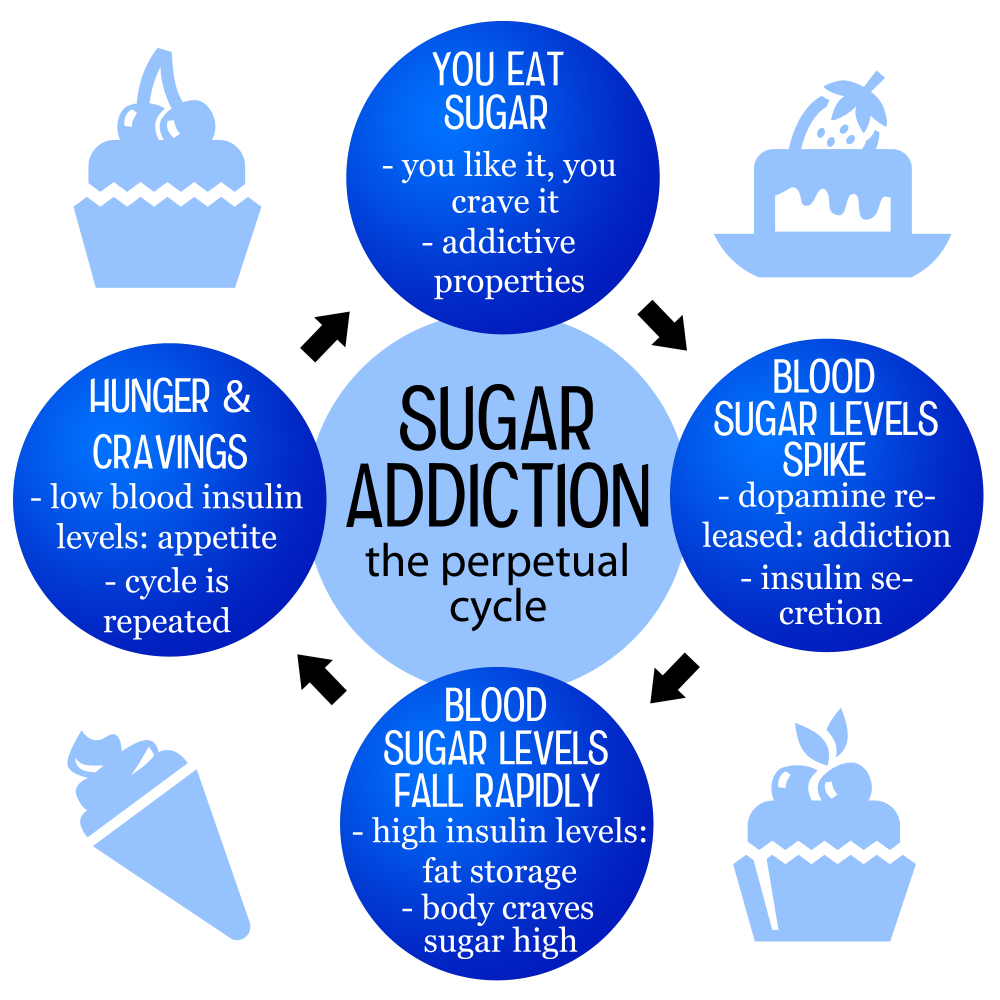
Is Sugar Addictive? Understanding the Cravings and Effects
Is sugar addictive? This question has sparked significant debate among nutrition researchers and health professionals alike. While substances like alcohol and nicotine fall squarely within the realm of addiction, sugar elicits strong cravings and compulsive behaviors that mimic addiction without meeting clinical definitions. The rise of processed foods, laden with added sugars, has made it easier for people to consume excessive amounts, leading to noteworthy health effects of sugar consumption. According to the American Heart Association sugar recommendations, excessive sugar intake can result in serious health complications, underscoring the need for awareness about our dietary choices and sugar cravings.
Exploring the potential addictive nature of sugar unveils a complex web of issues revolving around dietary habits and cravings. Terms like sweet dependency and sweet tooth often arise in discussions regarding our attraction to sugary foods, especially those found in highly processed items. These sugary substances, designed for maximum palatability, can trigger an intensely satisfying response, making it difficult to resist them. As individuals face escalating challenges with consumption, understanding the psychological and physiological implications of sugar addiction becomes crucial. By studying these relationships, we can garner insights into how to manage our intake and promote healthier eating behaviors.
Is Sugar Addictive? Understanding the Debate
The question of whether sugar is addictive has sparked considerable debate within the scientific community. While substances like alcohol and nicotine are classified as addictive substances due to their severe psychological and physiological effects, sugar does not fit neatly into this category. However, many individuals experience strong cravings for sugary foods, indicating that sugar does possess qualities that can lead to compulsive eating behaviors. Research has shown that sugar can activate the brain’s reward system, similar to other addictive substances, which complicates the conversation surrounding sugar addiction.
It is crucial to distinguish between physiological dependence and psychological cravings. Although some people may feel withdrawal-like symptoms when they reduce sugar intake, these effects tend to be milder than those associated with true addiction to drugs or alcohol. It’s the accessibility and appeal of sugar-laden, ultra-processed foods that make managing cravings challenging, leading to habitual consumption that can affect one’s health.
The contrasting viewpoints are important to consider when discussing the health effects of sugar. On one hand, moderate consumption is generally recognized as part of a balanced diet, but the overconsumption of added sugars can lead to negative health consequences such as obesity, diabetes, and cardiovascular disease. The American Heart Association recommends strict limits on added sugars—no more than 9 teaspoons for men and 6 teaspoons for women—to promote better health outcomes. Understanding that sugar is present in many nutrient-dense foods allows for a balanced view that supports moderation rather than total elimination.
The Impact of Sugar Cravings on Eating Habits
Sugar cravings can significantly influence an individual’s eating habits, often leading to the consumption of highly processed foods that are rich in added sugars. This change in dietary behavior can create a cycle of dependence, where the body craves more sugar to satisfy the initial desires, thus perpetuating the intake of unhealthy foods. These cravings can be particularly pronounced in times of stress, fatigue, or emotional distress, highlighting the psychological components tied to sugar consumption.
Research suggests that people who regularly consume high amounts of sugar are more likely to experience intense cravings, which can push them towards choosing sugary snacks over healthier options. This pattern is problematic, as it may lead to a cycle of unhealthy eating that is hard to break. Nutritional education, awareness, and mindful eating practices can help individuals recognize their cravings and make healthier choices without feeling deprived.
Furthermore, understanding the mechanism behind sugar cravings can empower individuals to make informed choices. Timing meals to include a balance of fiber, protein, and healthy fats can stabilize blood sugar levels and diminish the likelihood of sudden cravings. As lifestyle changes prove difficult, gradual reduction of added sugars in meals and snacks can help mitigate cravings without leading to overwhelming withdrawal-like symptoms. The goal should be to cultivate a health-focused environment that encourages mindful consumption and education about hidden sugars in processed foods.
Health Effects of Excess Sugar Consumption
The health effects of consuming excessive amounts of sugar are well-documented and extend beyond just weight gain. High sugar intake has been linked to various chronic diseases, including heart disease, diabetes, and fatty liver disease. Processed foods laden with sugars often lack essential nutrients, leading individuals to ingest empty calories that contribute to metabolic syndrome and obesity. This situation is compounded by the fact that many processed foods contain added sugars that go unrecognized by consumers, highlighting the necessity of reading food labels.
Moreover, the American Heart Association’s guidelines emphasize the long-term health risks associated with high sugar consumption. Limiting intake to recommended levels is key to reducing the risk factors associated with diet-related diseases. Understanding how much sugar is incorporated into daily foods allows for better dietary choices and supports public health initiatives aimed at reducing sugar consumption in the population.
In addition to physical health impacts, excessive sugar consumption can also affect mental well-being. Elevated blood sugar levels can lead to mood swings, fatigue, and an increased risk of depression. This relationship emphasizes the importance of considering both the psychological and physiological aspects of sugar intake and its cravings. By becoming more aware of sugar consumption and replacing unhealthy sugars with whole foods, individuals can enhance their overall health status and quality of life.
Navigating Sugar in a Processed Food World
In a world saturated with processed foods, navigating sugar consumption becomes a challenge for many individuals. Ultra-processed foods often contain high levels of added sugars, unhealthy fats, and sodium, making them exceptionally appealing and more likely to lead to overconsumption. This trend raises concerns over dietary habits and the public’s health as these foods contribute significantly to the average sugar intake, which currently exceeds the American Heart Association’s recommendations for added sugars.
To counteract this issue, consumers must develop skills in identifying sugar content in labels and making informed food choices. Engaging with whole foods and cooking meals from scratch can help mitigate the tendency towards grabbing sugary snacks, which are often designed for convenience rather than nutrition. Balancing the diet with fiber and nutrients while consciously reducing added sugars can lead to better health outcomes for individuals and families.
Furthermore, food manufacturers have a responsibility to reformulate their products and reduce added sugars to promote healthier options in the market. This shift requires collaboration between public health organizations and food producers to create a food environment that encourages healthy dietary patterns. By improving the accessibility of wholesome foods and enhancing nutrition education, we can support healthier eating habits and combat the rising prevalence of sugar-related health issues.
Combatting Sugar Addiction with Healthy Lifestyle Changes
Combatting sugar cravings and potential addiction necessitates a multifaceted lifestyle approach. One of the cornerstone strategies to reduce sugar intake effectively is through mindful eating practices. Individuals are encouraged to pay close attention to the types of foods consumed, focusing on natural sweeteners and whole foods that provide nourishment without the excessive sugar burden found in many snacks. These changes can lead to a more balanced consumption experience and reduce the overwhelming urge for sugary treats.
Incorporating regular physical activities can also help diminish sugar cravings. Exercise not only boosts mood and energy levels but also plays a significant role in regulating hormone levels that influence cravings. Engaging in moving activities encourages a healthier lifestyle overall and assists in offsetting the potential negative effects of occasional sugar indulgence.
Additionally, seeking support from professionals such as dietitians or nutritionists can provide tailored advice and strategies to help individuals manage their sugar cravings. These experts can assist in developing a personalized plan that aligns with one’s health goals, making the journey towards healthy eating both manageable and enjoyable. By fostering a supportive environment and building awareness around sugar consumption, individuals can cultivate a healthier relationship with food as they work towards reducing sugar’s presence in their diet.
Understanding the Role of Sweeteners in Our Diet
Understanding the role of sweeteners—both natural and artificial—in our diets is vital when discussing sugar addiction. While many seek to reduce their sugar intake, the market is flooded with alternatives, including stevia, agave nectar, and sugar alcohols. These sweeteners can satisfy cravings without the same caloric load or blood sugar impact, making them appealing for those looking to decrease their sugar consumption. However, it’s important to discern the health effects of these alternatives, as some may have their side effects or complicate the taste preferences that drive sugar consumption.
Moreover, the psychological impact of using substitutes can perpetuate sugar cravings rather than eliminate them. If individuals remain reliant on sweet tastes, they may struggle to achieve a balanced palate, leading to continued reliance on sweet foods and beverages. Comprehensively educating oneself about the profiles of various sweeteners and forming a preference for less sweetness can aid in reducing overall sugar dependency.
Ultimately, the goal should shift from merely avoiding sugar to fostering a holistic understanding of how different sweeteners play a role in overall health. This approach encourages consumers to experiment with various flavors and recognize that too much sweetness—regardless of the source—can lead to negative health consequences. By promoting awareness and reducing dependency on sweet flavors, individuals can foster a healthier relationship with food within the context of their dietary choices.
Tips for Gradually Reducing Sugar Intake
Making the decision to reduce sugar intake can feel overwhelming, but by taking gradual steps, this process can become much more manageable. One effective tip is keeping a food diary to track sugar consumption, which helps in identifying sources of added sugars in the diet. From sugary drinks to snacks, recognizing hidden sugars can empower individuals to make informed changes. This awareness can also help in setting realistic goals for reducing sugar without experiencing extreme cravings or discomfort.
Another strategy involves substituting sugary options with healthier alternatives. Rather than reaching for a candy bar, consider snacking on fruit or nuts, which can satisfy sweet cravings without the drawbacks of added sugars. Over time, these small changes can lead to a significant reduction in overall sugar intake, enhancing both health and well-being.
Finally, finding healthy ways to enjoy sweetness can also provide comfort while reducing dependence on high-sugar options. Integrating spices like cinnamon or vanilla extract can add a sweet flavor profile to dishes without the need for added sugars. This not only nurtures the satisfaction of taste but can also establish a new relationship with flavor in food—a relationship that emphasizes variety, balance, and health.
Frequently Asked Questions
Is sugar addictive like alcohol or nicotine?
While sugar can increase cravings and compulsive eating behaviors, it is not officially classified as an addictive substance like alcohol or nicotine. Current research suggests that though sugar has some addictive qualities, especially in the context of ultra-processed foods, it lacks the severe withdrawal symptoms associated with true addictive substances.
What causes sugar cravings and are they a sign of sugar addiction?
Sugar cravings can occur due to the palatable nature of sugary foods, often linked to habitual consumption. These cravings are intensified by processed foods high in sugar, unhealthy fats, and sodium. While these cravings can mimic signs of sugar addiction, they do not meet clinical criteria for addiction compared to substances like alcohol or nicotine.
What are the health effects of sugar consumption and should I be concerned?
Excessive sugar consumption can lead to a range of health issues, including obesity, diabetes, and heart disease. The American Heart Association recommends limiting added sugar to 9 teaspoons for men and 6 for women. Being mindful of sugar intake is crucial for maintaining overall health.
How can I reduce my sugar intake if I think I have a sugar addiction?
If you feel dependent on sugar, it’s advisable to gradually reduce your intake rather than going cold turkey, which can lead to withdrawal-like symptoms. Start by reading food labels, particularly on processed foods, and opt for healthier snacks with lower sugar content. This can help diminish sugar cravings over time.
What do the American Heart Association sugar recommendations suggest?
The American Heart Association recommends that men should limit their intake to no more than 9 teaspoons of added sugar per day, while women should consume no more than 6 teaspoons. Children should have even lower amounts, emphasizing the need to be aware of sugar consumption from processed foods and beverages.
Can sugar be part of a healthy diet without leading to addiction?
Yes, sugar can enhance flavor and texture in foods. It’s essential to distinguish between the natural sugars found in fruits and dairy versus added sugars in processed foods. Moderation is key; consuming low to moderate amounts of added sugar is usually safe and will not lead to significant health consequences.
Why are processed foods high in sugar so appealing and dangerous?
Processed foods are engineered to be highly palatable, containing added sugars that enhance flavor. This can lead to habitual eating patterns and heightened sugar cravings. The accessibility of these foods makes it challenging to limit intake, thus increasing potential health risks associated with overconsumption.
| Key Point | Details |
|---|---|
| Is Sugar Addictive? | Sugar is not classified as an addictive substance like alcohol or nicotine, according to current clinical criteria. |
| Physical and Psychological Effects | Sugar can increase cravings and compulsive eating, leading to withdrawal-like symptoms when stopped suddenly. |
| Ultra-Processed Foods | Foods high in added sugar, unhealthy fats, and sodium can exacerbate cravings due to their palatability. |
| Average Sugar Consumption | The average American consumes nearly 20 teaspoons of added sugar daily, far exceeding recommended limits. |
| Health Recommendations | American Heart Association recommends no more than 9 teaspoons for men, and 6 teaspoons for women. |
| Moderation is Key | Consuming sugar in moderation can enhance flavor and enjoyment, making it unnecessary to eliminate completely. |
Summary
Is sugar addictive? This question generates significant debate among nutritionists and researchers. While it shows addictive-like qualities in increasing cravings, sugar is not classified as an addictive substance like alcohol or nicotine based on strict clinical criteria. Unlike these substances, sugar is an essential part of our diet found in fruits and grains, suggesting we need a balanced approach to its intake. Therefore, understanding the impact of excessive sugar consumption and moderating its use can help avoid potential negative psychological effects while still enjoying its benefits.

Indoor Air Quality: How It Affects Your Health Now
Indoor air quality is a critical aspect that significantly impacts our health and overall well-being. In fact, the health effects of indoor air quality can range from mild symptoms like fatigue and concentration issues to more severe respiratory problems. Understanding the importance of ventilation is vital, as proper airflow can help to reduce indoor air pollutants that accumulate in our living and working spaces. Studies suggest that improving indoor air quality can lead not just to healthier buildings, but also to enhanced cognitive function and productivity. As we explore this topic further, the link between our environments and our physical health becomes increasingly evident.
When discussing the quality of air within buildings, we often underscore the effects it has on our physical health and daily functionality. The environments we inhabit—be it at home, in offices, or in educational settings—play a crucial role in determining how we feel and perform. Ensuring proper ventilation helps mitigate harmful airborne contaminants that can adversely affect our well-being. Additionally, a focus on establishing healthy indoor spaces can lead to substantial improvements in life quality and productivity. As we delve deeper into this subject, we will uncover various strategies for enhancing the air we breathe indoors.
Understanding Indoor Air Quality and Its Health Effects
Indoor air quality (IAQ) is a critical aspect of health that often goes unnoticed until it leads to tangible effects. Poor IAQ can have serious implications on physical health, contributing to conditions such as respiratory diseases, allergies, and even cardiovascular issues. The presence of common indoor air pollutants like mold, carbon dioxide, volatile organic compounds (VOCs), and particulate matter can compromise the environment in which we live and work, highlighting the urgent need to assess and improve indoor environments.
Moreover, the health effects of indoor air quality extend beyond physical ailments. Psychological impacts due to ongoing discomfort from poor air quality can lead to decreased productivity and increased stress levels. Studies have shown that individuals working in well-ventilated spaces with high IAQ report better cognitive function and mood, reinforcing the link between indoor conditions and overall well-being. Understanding this relationship empowers us to take necessary actions to enhance our indoor spaces and mitigate health risks.
Frequently Asked Questions
What are the health effects of indoor air quality?
Indoor air quality significantly impacts health. Poor air quality can lead to respiratory issues, headaches, fatigue, and can exacerbate allergies and asthma. Long-term exposure to indoor air pollutants may result in chronic health conditions.
Why is the importance of ventilation in maintaining indoor air quality?
Ventilation is crucial because it helps dilute indoor air pollutants and bring in fresh air. Proper ventilation reduces the concentration of harmful substances, improves overall air quality, and supports a healthier living environment.
How do healthy buildings impact indoor air quality?
Healthy buildings are designed with features that enhance indoor air quality, such as effective ventilation systems, use of non-toxic materials, and air filtration. These features can reduce pollutants and allergens, promoting better health and productivity.
What are some common indoor air pollutants that affect air quality?
Common indoor air pollutants include mold, dust mites, pet dander, volatile organic compounds (VOCs), and carbon monoxide. These pollutants can affect health and are often found in various household products and materials.
What are effective ways to improve indoor air quality?
Improving indoor air quality can be achieved by increasing ventilation, using high-efficiency air filters, reducing the use of VOCs and toxic chemicals, regularly cleaning and maintaining HVAC systems, and incorporating plants that help purify the air.
| Key Area | Details |
|---|---|
| Indoor Air Quality | Indoor air quality significantly impacts health, including cognitive functions and overall well-being. |
| Average Time Indoors | Americans spend about 80% of their lives indoors. |
| Effect of Ventilation | Increasing building air ventilation has been shown to improve cognitive function. |
| Source of Air Pollution | Indoor spaces can be a source of outdoor air pollution. |
| Impact of Neighboring Units | In an apartment, up to 30% of indoor air can come from neighboring units. |
| Infectious Disease Prevention | To reduce indoor spread of diseases, increase outdoor air, use better filters, and deploy HEPA filters. |
| Dust Composition | Dust can be hormonally active. |
| Chemical Regulations | Only about 200 out of 80,000+ chemicals have been banned by the EPA since 1976. |
Summary
Indoor air quality plays a crucial role in our health and well-being, influencing both cognitive function and overall wellness. As our lives are predominantly spent indoors, attention must be directed toward how buildings are designed and maintained to ensure adequate ventilation and minimize exposure to harmful pollutants. By improving indoor air quality through better ventilation, filtration, and awareness of pollutants, we can significantly enhance our work and living environments.

AI in Healthcare: Transforming Patient Care with Technology
AI in healthcare is revolutionizing the medical landscape, promising unprecedented improvements in patient outcomes and operational efficiency. The integration of artificial intelligence into medicine has led to a surge in AI medical applications that enhance the accuracy of diagnoses and treatment plans. With healthcare AI benefits such as reduced administrative burdens and better access to patient information, the technology is reshaping how doctors interact with patients. For instance, large language models in medicine are now capable of synthesizing vast amounts of medical literature in real-time, transforming the doctor-patient dialogue. However, despite the potential for AI to bridge healthcare disparities, developers must navigate the complexities of bias in data to ensure equitable care for all patients.
The emergence of advanced technology in medical care, particularly intelligent systems that can analyze and interpret complex data, marks a significant shift in healthcare practices. Many professionals are now exploring how computational models and machine learning can aid in clinical decision-making and improve patient care processes. These transformative tools promise to enhance the efficiency of medical services, providing timely and personalized treatment options. Moreover, as we delve into this new era, the importance of addressing issues related to AI and healthcare disparities cannot be overlooked, as it is crucial for ensuring that these innovations benefit everyone, regardless of socioeconomic status.
The Transformative Power of AI in Healthcare
Artificial Intelligence (AI) is changing the landscape of healthcare, offering innovative solutions that significantly improve patient care and operational efficiency. With advancements in machine learning and data analysis, AI medical applications are streamlining processes that previously consumed significant time and resources. A prime example is the integration of large language models, like OpenEvidence, which allow clinicians to access and process vast amounts of medical literature in milliseconds. This capability not only enhances decision-making but also equips healthcare professionals to deliver evidence-based care more swiftly, thereby improving patient outcomes.
Moreover, the benefits of healthcare AI extend beyond mere efficiency. The use of AI can potentiate personalized medicine, helping to tailor treatments based on individual patient data. By analyzing patterns across numerous cases, AI systems can identify specific needs and potential responses to various therapies, leading to more effective interventions. This personalized approach not only improves treatment efficacy but also increases patient satisfaction and trust in the healthcare system.
Mitigating Healthcare Disparities through AI Technologies
A critical issue within healthcare today is the presence of disparities that affect marginalized populations. AI solutions hold the potential to reduce these disparities by harnessing data-driven insights to identify gaps in care delivery. For instance, language models in medicine can analyze patient records and highlight underrepresented groups in clinical trials, ensuring that research outcomes are more applicable to diverse populations. This focus on inclusivity may significantly enhance the quality of care for patients who have traditionally faced obstacles in accessing appropriate medical services.
Furthermore, AI can help refine existing healthcare algorithms to avoid unintentional biases. By utilizing large datasets that include diverse demographics, AI applications can be designed to ensure equitable outcomes in treatment and diagnosis. Such adjustments could lead to an improved understanding of how various factors, such as socioeconomic status and language proficiency, influence healthcare access and quality. Addressing these disparities is crucial, as it aligns with ethical considerations and contributes to a fairer healthcare system that benefits all segments of society.
AI-Driven Innovations in Medical Education
The integration of artificial intelligence in medical education is paving the way for a new generation of healthcare professionals. Training programs are increasingly incorporating AI tools to enhance learning experiences and facilitate deeper cognitive understanding of complex medical concepts. For example, the development of AI tutoring systems provides personalized feedback and resources to students, helping them grasp intricate topics more effectively than traditional methods allow.
Additionally, the use of AI in simulating patient interactions offers medical students the chance to practice diagnosing and managing conditions in a risk-free environment. This hands-on approach builds confidence and skills, preparing students for real-life clinical situations. By embracing AI tools, educational institutions can cultivate future healthcare leaders who are adept at using technology to improve patient care and embrace continuous learning.
Enhancing Patient Safety through AI Solutions
AI technologies are proving to be instrumental in enhancing patient safety within healthcare settings. With the ability to analyze extensive data sets, AI can identify potential risks associated with drug interactions, adverse reactions, and procedural errors. For example, AI systems can monitor medication administration to ensure that patients receive the correct dosages and alert healthcare providers about possible interactions before they occur. This capability not only decreases the likelihood of harmful events but also promotes a culture of safety in medical practice.
Moreover, implementing AI-driven tools can lead to better identification and management of conditions that are prone to oversight. AI models can analyze clinical data and present potential diagnoses that may have been overlooked by human practitioners. This collaborative approach allows healthcare professionals to validate their assessments while being aware of other possibilities, ultimately assisting in more accurate diagnoses and treatment plans.
Ethical Considerations in AI Implementation
As artificial intelligence continues to transform healthcare, ethical considerations regarding its implementation must be addressed. Healthcare providers must navigate the complexities of data privacy, informed consent, and the potential for algorithmic bias. To ensure that AI in healthcare serves the best interests of patients, practitioners and developers must prioritize transparency in how AI systems function and make decisions, particularly in sensitive areas such as patient diagnostics and treatment recommendations.
Furthermore, it is crucial to actively work against existing biases in data that could exacerbate healthcare disparities. Researchers must ensure diverse representation in datasets used to train AI systems to create algorithms that better serve all populations. Engaging various stakeholders in the healthcare ecosystem, including ethicists, patients, and community advocates, can foster an inclusive dialogue that shapes the ethical framework guiding AI applications in medicine.
The Role of AI in Streamlining Administrative Tasks
Administrative burden has become a challenge facing healthcare professionals, detracting from time spent with patients. AI applications can alleviate some of this burden by automating routine tasks such as appointment scheduling, billing, and documentation. This level of automation not only reduces human error but also allows healthcare workers to dedicate more time to patient care, ultimately enhancing the quality of interactions between staff and patients.
Additionally, AI systems can analyze patient flow and operational workflows within healthcare facilities to identify inefficiencies. By optimizing schedules and resource allocation, healthcare providers can enhance service delivery, resulting in improved patient experiences and more efficient use of resources. This holistic approach to administrative management offers long-term benefits for the healthcare system, including cost savings and better resource stewardship.
AI-Powered Predictive Analytics for Better Outcomes
Predictive analytics powered by AI is changing the way healthcare providers approach patient care. By analyzing historical patient data, AI algorithms can forecast trends and outcomes, allowing for proactive management of diseases. For instance, using machine learning to predict the onset of diseases among at-risk populations enables early intervention strategies, which can be more effective and less costly than reactive treatments.
These predictive capabilities extend to resource allocation as well. For example, AI can help hospitals predict patient admission rates, which allows for better staffing and resource management. This not only improves operational efficiency but also directly impacts patient outcomes by ensuring that sufficient resources are available when needed. The culmination of these efforts fosters a more responsive healthcare system that is better equipped to meet the evolving needs of patients.
The Future of AI in Medical Research
As the field of medical research evolves, AI is enhancing the speed and accuracy of discoveries. AI tools facilitate the analysis of vast datasets, enabling researchers to uncover insights that would be time-prohibitive through traditional methods. This capability is particularly impactful in drug discovery, where AI can predict how new compounds may interact with biological targets, expediting the development process and reducing costs.
Moreover, AI assists in identifying gaps in current research, guiding scientific inquiry toward pressing health issues that require attention. By analyzing past research outcomes and current trends, AI can highlight areas where innovation is desperately needed, ensuring that future research efforts are directed toward the most consequential public health challenges. This strategic alignment of research objectives with AI insights has the potential to vastly improve health outcomes on a global scale.
The Intersection of AI and Telemedicine
The rise of telemedicine has been significantly augmented by AI, bringing healthcare services to the forefront of remote accessibility. AI-enabled telehealth platforms are capable of triaging cases, suggesting appropriate care pathways, and facilitating virtual consultations between providers and patients. This capability is particularly notable in areas with underserved populations, as it ensures timely access to medical expertise, regardless of geographical constraints.
Furthermore, AI enhances the efficiency and accuracy of telemedicine by automating routine processes such as patient intake and follow-up reminders. By freeing healthcare providers from administrative tasks, telemedicine becomes a more effective tool for reaching patients, allowing providers to focus wholly on delivering care. This integration not only improves healthcare outcomes, but also contributes to patient retention and satisfaction in an increasingly digital age.
Frequently Asked Questions
What are the benefits of AI in healthcare?
AI in healthcare brings numerous benefits, including improved diagnostic accuracy, personalized treatment plans, and enhanced patient care efficiency. By utilizing AI medical applications, healthcare providers can analyze vast amounts of data rapidly, leading to quicker and more accurate decisions. Additionally, AI reduces administrative burdens on clinicians, allowing them to focus more on patient interaction and care.
How does artificial intelligence improve medical diagnoses?
Artificial intelligence enhances medical diagnoses by employing large language models and machine learning algorithms to analyze patient data and medical literature. AI algorithms can quickly identify patterns and correlations that may be missed by human clinicians, thus providing more accurate and timely diagnostic suggestions, especially in complex cases.
What role do language models play in medicine?
Language models in medicine, such as GPT-4, assist healthcare professionals by processing vast amounts of medical information and generating insightful summaries. These models can answer specific medical questions, suggest possible diagnoses, and provide treatment recommendations, thereby improving the efficiency of doctor-patient interactions and supporting clinical decision-making.
How does AI help address healthcare disparities?
AI has the potential to address healthcare disparities by providing greater access to quality care for underserved populations. By leveraging AI medical applications, healthcare systems can analyze data to identify gaps in services and target interventions more effectively. However, it is crucial to ensure that the AI systems are trained on diverse datasets to avoid perpetuating existing biases.
What challenges are associated with AI in healthcare?
Despite its promise, AI in healthcare faces challenges, including potential biases in data, the risk of AI hallucinations (false information generation), and concerns about over-reliance on technology at the expense of medical training. To maximize the benefits of AI, it is essential to monitor its implementation and refine AI systems continuously to ensure they improve healthcare outcomes.
| Key Points | Details |
|---|---|
| AI in Healthcare | AI technologies are poised to significantly transform healthcare by improving efficiency, reducing errors, and enhancing patient interactions. |
| Impact on Medical Practice | AI can assist doctors in diagnostics, integrate data for better decision-making, and alleviate administrative burdens, allowing for deeper patient interactions. |
| Education and Training | Emerging AI tools can improve medical education by providing students with simulation opportunities and enhancing learning through access to vast medical literature. |
| Ethical Concerns | AI inherits biases from existing data sets, potentially perpetuating disparities in healthcare access and quality. |
| Future Potentials | AI could lead to innovative solutions, including real-time patient monitoring and personalized treatment plans. |
Summary
AI in healthcare represents a groundbreaking evolution in medical practices, promising to enhance the efficiency and quality of patient care through more informed decision-making and streamlined processes. As we explore the integration of AI in medicine, it is crucial to address the ethical implications and inherent biases within AI systems to ensure equitable healthcare for all. The future of AI in healthcare looks bright, filled with opportunities to advance medical education and elevate the standards of patient interactions.
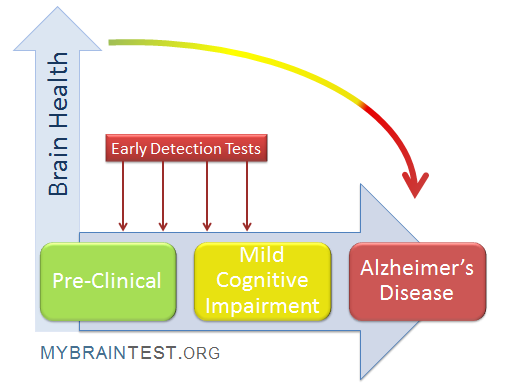
Alzheimer’s Early Detection: Innovative Home Testing Methods
Alzheimer’s early detection is crucial in the fight against this debilitating disease, and new research sheds light on innovative methods to identify at-risk individuals before significant symptoms arise. A groundbreaking study by researchers at Mass General Brigham reveals that an easy, at-home olfactory test could serve as an effective tool for assessing cognitive impairment. This test allows participants to evaluate their ability to discriminate, identify, and remember odors, providing a noninvasive way to pinpoint early signs of Alzheimer’s disease and other neurodegenerative diseases. Notably, the findings indicate that older adults with cognitive impairment consistently scored lower than their cognitively healthy peers, highlighting the potential of olfactory dysfunction as a warning sign. As we delve deeper into Alzheimer’s research, these discoveries could pave the way for earlier interventions and improved treatment options.
Identifying subtle indicators of cognitive decline is gaining traction, particularly through novel home testing approaches. Recent advancements in this field explore the relationship between smell and memory, showing that individuals may reveal early signs of neurodegenerative conditions through olfactory assessments. These developments could be game-changers for early diagnosis, especially for conditions like Alzheimer’s disease. By leveraging simple tests that assess odor recognition and memory, researchers aim to unveil potential cognitive issues long before noticeable symptoms develop. This early detection not only enhances understanding of cognitive health but also sets the stage for timely therapeutic interventions.
The Importance of Early Detection in Alzheimer’s Disease
Early detection of Alzheimer’s disease is crucial for effective intervention and management, as it allows for timely treatment that may slow the progression of the disease. Studies indicate that identifying cognitive impairment early on can enhance patients’ ability to maintain independence for a longer period. Researchers emphasize the role of olfactory testing in this early detection process, showing that a simple smell test can reveal signs of cognitive decline before more severe symptoms develop. This innovative approach aligns with the shift towards preventive healthcare, focusing on identifying risk factors to prevent or delay the onset of neurodegenerative diseases.
Furthermore, the integration of home testing solutions offers patients a convenient way to monitor their cognitive health. With advancements in technology, olfactory tests can now be administered at home, empowering individuals to take charge of their health. These tests can help bridge the gap in clinical settings where professional evaluations may not be readily available, especially in under-resourced areas. Thus, as Alzheimer’s research continues to evolve, the application of at-home cognitive assessments is positioned to play a vital role in routine health checkups, making early detection accessible and practical.
Frequently Asked Questions
What role does olfactory testing play in Alzheimer’s early detection?
Olfactory testing is a promising method for Alzheimer’s early detection as research indicates that a decline in odor identification can signal cognitive impairment. Participants who performed lower in olfactory tests are more likely to be at risk for neurodegenerative diseases such as Alzheimer’s, allowing for interventions years before memory symptoms appear.
How can cognitive impairment be assessed for Alzheimer’s early detection?
Cognitive impairment can be assessed through various tests, including olfactory tests that evaluate a person’s ability to identify and discriminate odors. These tests can indicate the risk of Alzheimer’s disease and are effective even when conducted as at-home tests, making them convenient for early detection.
Are there home testing options for Alzheimer’s early detection?
Yes, there are home testing options available for Alzheimer’s early detection, particularly olfactory tests. These tests allow individuals to assess their olfactory abilities and detect early signs of cognitive decline without needing to visit a clinic, promoting early intervention strategies.
What advancements are being made in Alzheimer’s research regarding early detection?
Recent advancements in Alzheimer’s research focus on olfactory testing as a noninvasive method for early detection of cognitive impairment. Studies show that measuring an individual’s ability to identify and remember odors provides valuable insights into their risk for developing Alzheimer’s and other neurodegenerative diseases.
How is the Aromha Brain Health Test utilized in Alzheimer’s early detection?
The Aromha Brain Health Test is used in Alzheimer’s early detection by measuring participants’ odor discrimination and recognition abilities. Researchers have found that lower scores on this olfactory test correlate with cognitive impairment, making it a useful tool for identifying individuals at risk of Alzheimer’s before clinical symptoms emerge.
Why is olfactory dysfunction considered a warning sign for Alzheimer’s?
Olfactory dysfunction, characterized by a reduced ability to detect and identify smells, has been linked to neurodegenerative diseases such as Alzheimer’s. This association suggests that changes in smell can be early indicators of cognitive decline, signaling a potential risk for developing Alzheimer’s disease.
What are the benefits of conducting Alzheimer’s early detection tests at home?
Conducting Alzheimer’s early detection tests at home, like olfactory tests, enhances accessibility and encourages more individuals to participate in screening. This convenience can lead to increased awareness of cognitive health, enabling timely intervention and management of neurodegenerative diseases.
What findings support the use of olfactory tests for Alzheimer’s early detection?
Findings from recent studies reveal that older adults with cognitive impairment scored significantly lower on olfactory tests compared to cognitively normal individuals. This decline in odor identification and discrimination indicates that olfactory testing could reliably serve as an early detection method for Alzheimer’s and related cognitive disorders.
Can olfactory tests predict future cognitive decline related to Alzheimer’s disease?
Yes, olfactory tests can potentially predict future cognitive decline associated with Alzheimer’s disease. Research indicates a consistent correlation between poor performance on these tests and the likelihood of developing Alzheimer’s symptoms, making olfactory assessments a key focus in early detection strategies.
| Key Point | Details |
|---|---|
| At-home olfactory tests | New tests help identify those at risk of Alzheimer’s years before symptoms appear. |
| Importance of early detection | Early detection of cognitive impairment can allow for timely interventions. |
| Participants tested | Included older adults with cognitive complaints and those with mild cognitive impairment. |
| Findings | Lower scores in odor discrimination and identification in cognitively impaired adults compared to normal. |
| Cross-linguistic assessment | Test results were consistent among English- and Spanish-speaking participants. |
| Future research directions | Further studies could combine neuropsychological testing to predict cognitive decline over time. |
Summary
Alzheimer’s early detection plays a crucial role in the management and treatment of cognitive impairment. The innovative research conducted by scientists from Mass General Brigham highlights the potential of at-home olfactory tests to reveal risk factors for Alzheimer’s years before the onset of noticeable symptoms. By utilizing simple smell tests, this groundbreaking approach not only paves the way for effective early identification but also underscores the importance of seeking timely interventions. As we advance in understanding neurodegenerative diseases, tools like olfactory testing could revolutionize early diagnosis and treatment strategies for Alzheimer’s.

Industrial Chemicals Effects: Protecting Human Health
Industrial chemicals effects are becoming a growing concern in our increasingly chemical-dependent world, impacting both human health and environmental safety. Each day, countless products we utilize, from clothing to electronics, are fabricated using a myriad of chemicals, many of which pose serious chemical hazards. Understanding the implications of these substances is crucial, as they can adversely affect not only individuals but also ecosystems. To address these challenges, organizations like ChemFORWARD strive to compile a safe chemicals database that offers insights into the toxicology assessments of various industrial chemicals. Through this effort, they aim to mitigate the environmental health risks associated with harmful chemicals, ultimately promoting safer alternatives that protect our society and planet.
The effects of industrial chemicals, often referred to as chemical impacts, encompass a range of health and environmental concerns stemming from the widespread use of hazardous materials in production processes. As society becomes increasingly aware of the potential dangers associated with certain human health chemicals, initiatives focused on cataloging and assessing these substances grow in importance. By harnessing comprehensive data on toxicological profiles and environmental implications, organizations can help navigate the complex landscape of chemical safety. This proactive approach enables consumers and industries alike to make informed choices, reducing the risk of exposure to harmful agents while fostering a healthier, more sustainable future.
Understanding Chemical Hazards in Everyday Products
Chemical hazards are present in many of the products we use daily, often unbeknownst to the average consumer. Items ranging from clothing and furniture to personal care products contain a multitude of chemicals that can pose significant health risks. For instance, certain synthetic dyes used in fabrics have been linked to skin irritations and even carcinogenic properties. This underscores the importance of being aware of the chemical cocktail that resides in our homes and on our bodies.
Organizations like ChemFORWARD play a crucial role in educating consumers and companies about these chemical hazards. By providing a comprehensive database and chemical hazard assessments, they empower stakeholders to make informed decisions regarding the safety of products. This proactive approach not only helps in minimizing exposure to harmful chemicals but also contributes to a greater understanding of the potential long-term health implications.
The Impact of Industrial Chemicals on Human Health
Industrial chemicals have far-reaching effects on human health, impacting various systems within the body. Chemicals used in the manufacturing of products, such as flame retardants and plastics, can lead to serious health challenges, including endocrine disruption and reproductive issues. Understanding the specific health impacts associated with these substances is vital for consumers, especially when choices are made without full knowledge of the chemical compositions involved.
Through initiatives such as ChemFORWARD, companies are urged to utilize verified chemical hazard assessments that consider a range of health endpoints. This data-driven approach is essential in identifying chemicals that pose significant risks to human health, enabling businesses to make safer product choices. As awareness grows about the dangers of these industrial chemicals, consumers are increasingly demanding transparency and safer alternatives.
Environmental Health Risks from Chemicals
The environmental health risks from industrial chemicals are escalating concerns that can no longer be overlooked. Chemicals released during production processes can contaminate soil and water, contributing to ecosystem disturbances and harming wildlife. Substances such as heavy metals and persistent organic pollutants can stay in the environment for years, accumulating in the food chain and posing risks to both human and environmental health.
By fostering collaboration between industries and environmental organizations, the impact of these pollutants can be mitigated. Organizations like ChemFORWARD serve as a bridge, bringing together businesses that wish to reduce their environmental footprint with robust data on chemical safety. Their work highlights the need for sustainable practices that protect both public health and the environment.
Utilizing Safe Chemicals Databases for Better Practices
The advent of safe chemicals databases marks a turning point in how industries approach chemical safety. Such resources allow companies to access verified information about the hazards associated with various chemicals, thereby facilitating safer decision-making in product development. By relying on databases like ChemFORWARD, businesses can identify alternatives to harmful substances and prioritize those that pose minimal risks to human and environmental health.
The integration of safety databases into corporate processes not only enhances product safety but also fosters consumer trust. As more companies adopt these practices, it sets a precedent for the industry to prioritize sustainability and health. This shift is essential as consumers grow more conscious of the products they use and the implications those products have on their health and the world around them.
Toxicology Assessments and Their Role in Product Safety
Toxicology assessments are crucial tools in determining the safety of chemicals used in various products. By evaluating the potential health effects of substances, these assessments help identify risks related to exposure, including carcinogenicity, mutagenicity, and reproductive toxicity. With comprehensive toxicological data, companies can develop safer products and minimize adverse health effects on consumers.
Furthermore, transparency in toxicological assessments empowers consumers to make informed choices about the products they purchase. Organizations like ChemFORWARD provide accessible assessments that facilitate understanding of the risks associated with specific chemicals. This initiative encourages both businesses and consumers to prioritize safety and health in their buying decisions.
The Role of Industry Collaboration in Reducing Chemical Hazards
Collaboration across industries is imperative for reducing chemical hazards and promoting public health. Companies that share data and resources can collectively advance the safety of products in the marketplace. For instance, partnerships with organizations like ChemFORWARD allow businesses to draw from a shared pool of chemical hazard assessments, improving the overall safety standards across sectors and enhancing the public’s trust in product safety.
Such collaborations are not just beneficial for individual companies; they also contribute to shaping industry-wide practices that prioritize human health and environmental sustainability. As companies begin to recognize the importance of collaboration in addressing chemical hazards, it sets a powerful precedent for collective action in promoting safer chemical practices.
Navigating Chemical Regulations in a Complex Landscape
Navigating the landscape of chemical regulations can be daunting for companies, particularly those aiming to ensure product safety and compliance. Regulations vary widely across regions and industries, and the lack of a universal standard often leads to confusion. Organizations such as ChemFORWARD help bridge this gap by offering resources that clarify regulatory requirements and streamline compliance with safety standards.
Understanding these regulations is critical not only for legal compliance but also for achieving greater safety in product formulations. Companies that actively engage in regulatory dialogues and adjust their practices accordingly can better position themselves as leaders in safety and sustainability, ultimately benefiting consumer health and environmental integrity.
The Future of Chemical Safety: Innovations and Trends
The future of chemical safety is on the verge of transformation, driven by innovations and increased public awareness. As demand for safer products grows, companies are investing in research and development to create non-toxic alternatives to traditional chemicals. This trend is underpinned by a broader movement towards sustainability and a deeper understanding of the impacts of chemical exposure on human health and the environment.
Advancements in technology, such as artificial intelligence and big data analytics, are also shaping the future of chemical safety. These tools can analyze vast amounts of data regarding chemical hazards and assist companies in making informed decisions about product formulations. This evolution in risk assessment processes will likely lead to safer products entering the market, ultimately benefiting both consumers and the environment.
Educating Consumers on Chemical Safety
Consumer education is essential in fostering awareness about chemical safety and the hazards associated with everyday products. Many people remain unaware of the potential risks chemical components pose, which can lead to unsafe consumption patterns. Organizations like ChemFORWARD are taking the lead in providing resources that inform consumers about the chemicals present in the products they use, enabling them to make safer choices.
By empowering consumers with knowledge about harmful substances, awareness can drive demands for safer alternatives. This shift not only influences purchasing behaviors but also compels manufacturers to prioritize safety in product development. As the demand for transparency in the safety of chemicals continues to rise, educating consumers will play a critical role in shaping the market.
Promoting Safer Products Through Chemical Assessments
Chemical assessments serve as a vital tool in promoting the development of safer products. By systematically evaluating chemicals used in manufacturing, companies can identify those that pose significant health risks and replace them with safer alternatives. Programs like ChemFORWARD offer valuable assessments that allow organizations to make decisions grounded in data, fostering a culture of responsibility and care in product safety.
As this assessment culture grows within industries, the overall market trend is toward greater accountability regarding chemical use. Companies are not just focused on compliance; they are embracing the responsibility to protect public health and sustainability. The importance of these assessments cannot be overstated, as they lay the foundation for innovation and safe product design in a chemical-heavy world.
Frequently Asked Questions
What are the human health effects of industrial chemicals according to toxicology assessments?
Toxicology assessments indicate that numerous industrial chemicals can negatively impact human health. These effects include carcinogenicity, mutagenicity, reproductive toxicity, neurotoxicity, and various forms of irritation (skin and eye). Understanding these effects helps us identify chemical hazards and make informed choices to protect ourselves and our families.
How do industrial chemicals affect environmental health risks?
Industrial chemicals contribute to environmental health risks by introducing toxic substances into ecosystems. These chemicals can persist in the environment, impacting wildlife and natural resources, and can also contaminate food and water supplies. Assessments of these chemicals help in evaluating their long-term effects on both human health and environmental stability.
What resources are available for accessing a safe chemicals database?
One prominent resource is the ChemFORWARD database, which comprises a repository of verified chemical hazard assessments. This database provides valuable information for companies seeking to reduce the use of harmful chemicals in their products and supply chains, ensuring better safety for both human health and the environment.
Why is it important to assess chemical hazards in industrial settings?
Assessing chemical hazards in industrial settings is crucial to identify potential risks associated with the chemicals used in manufacturing processes. This proactive approach not only helps protect workers’ health but also mitigates environmental impacts, ensuring compliance with safety regulations and promoting sustainable practices.
What is the relationship between chemical hazards and consumer products?
Consumer products often contain industrial chemicals that may pose health risks. Understanding the chemical hazards associated with these substances is vital for making safer consumer choices. Initiatives like ChemFORWARD aim to inform consumers and manufacturers about the health impacts of these chemicals, promoting transparency and safety in the marketplace.
How can companies utilize toxicology assessments to improve product safety?
Companies can leverage toxicology assessments to identify and mitigate the risks associated with the chemicals they use. By integrating findings from these assessments into their product design and supply chain management, businesses can create safer products, comply with health regulations, and build consumer trust.
What role do regulatory frameworks play in managing industrial chemicals?
Regulatory frameworks establish guidelines for assessing and managing the risks associated with industrial chemicals. These regulations, such as the EU’s REACH program, require companies to evaluate chemical safety, thereby minimizing health and environmental risks from potential chemical hazards.
How can the data from safe chemicals databases be leveraged for research purposes?
Data from safe chemicals databases, like ChemFORWARD, can be instrumental for researchers monitoring chronic health effects or environmental impacts. This accessible information enables cross-sector collaboration and supports the development of safer chemicals and sustainable practices.
| Key Points | Details |
|---|---|
| ChemFORWARD Introduction | ChemFORWARD has developed a database of industrial chemicals to promote safer products by assessing their effects on human and environmental health. |
| Award Recognition | ChemFORWARD received the Roy Family Award for Environmental Partnership from Harvard Kennedy School for its innovative approach to chemical safety. |
| Chemical Hazard Assessments (CHAs) | The database includes verified assessments that help companies make informed decisions about chemical use in their supply chains. |
| Need for Chemical Vetting | There are currently no universal requirements to vet all industrial chemicals before they are used in products, leading to potential health risks. |
| Environmental and Human Health Assessments | ChemFORWARD evaluates chemicals for various health risks including carcinogenicity and reproductive toxicity, as well as environmental persistence. |
| Impact on Collaboration | Companies like Google collaborate with ChemFORWARD to enhance product safety and share valuable hazard assessment data. |
Summary
Industrial chemicals effects are a significant concern for both public health and environmental sustainability. The risks posed by hazardous chemicals found in everyday products can lead to serious health issues, affecting everyone from consumers to workers in manufacturing sectors. Organizations like ChemFORWARD are pioneering efforts to catalogue and assess these chemicals, providing vital information that helps companies minimize their impact on human health and the environment. By promoting transparency and collaboration, these initiatives strive to create safer, healthier products for society.